YOUR JOURNEY TO ORAL HEALTH IS A COLLABORATIVE AND TRANSPARENT EXPERIENCE.

Embrace Integrity

Foster Personal Connections

Achieve Outstanding Results
OUR SERVICES
At Smile Esthetics, we are a family-centric dental office in Scottsdale specializing in family and cosmetic dentistry. As you will see below, we offer many other dental services in addition to routine checkups and cleanings, including dental crowns, which are a type of dental restoration that is used to protect your natural teeth and strengthen them. Partial dentures are used to replace missing teeth and provide a more natural look. Cosmetic dentistry is an esthetic approach to the patient’s health and well-being. Not only do we focus on the shapes and shades of your teeth but also on the functionality. Teeth whitening is a safe and effective way to get a brighter smile. Veneers are a popular dental procedure that can improve the appearance of your teeth. They can be made of zirconia, lithium disilicate or porcelain and are custom-designed to fit your smile, so they look natural and feel completely comfortable. You can always count on us for your routine visits and emergency dental care. Our Scottsdale dentist, Dr. Mariana Conant, and her staff take pride in being there for you when you need them most. We hope that your visits with us are enjoyable, and we thank you for considering our services.
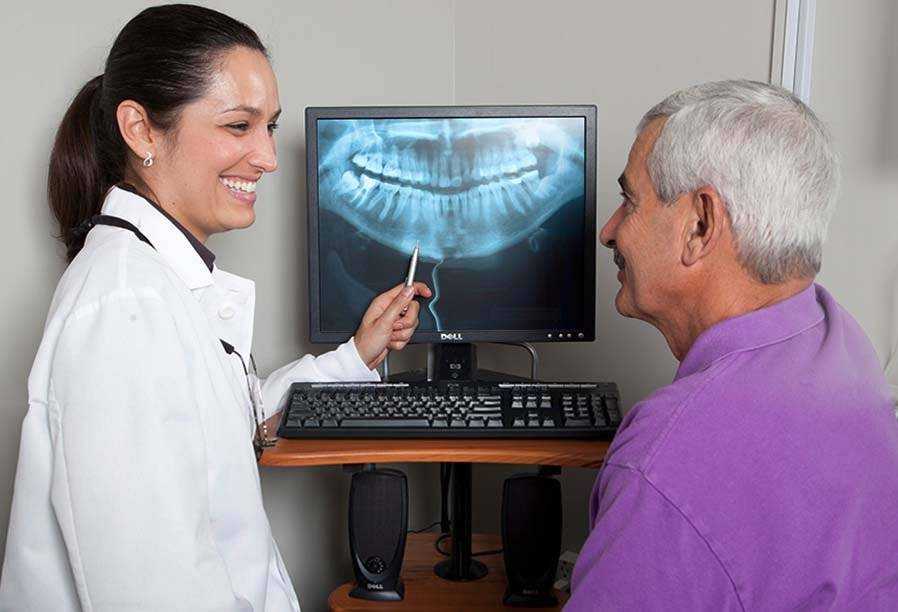
Dental Care
Dental exams and cleanings are routine checkups that deal with a person’s mouth, teeth, and overall oral health.
Dental Implants
If you have missing teeth and are looking for an option for replacing them, you should think about dental implants.
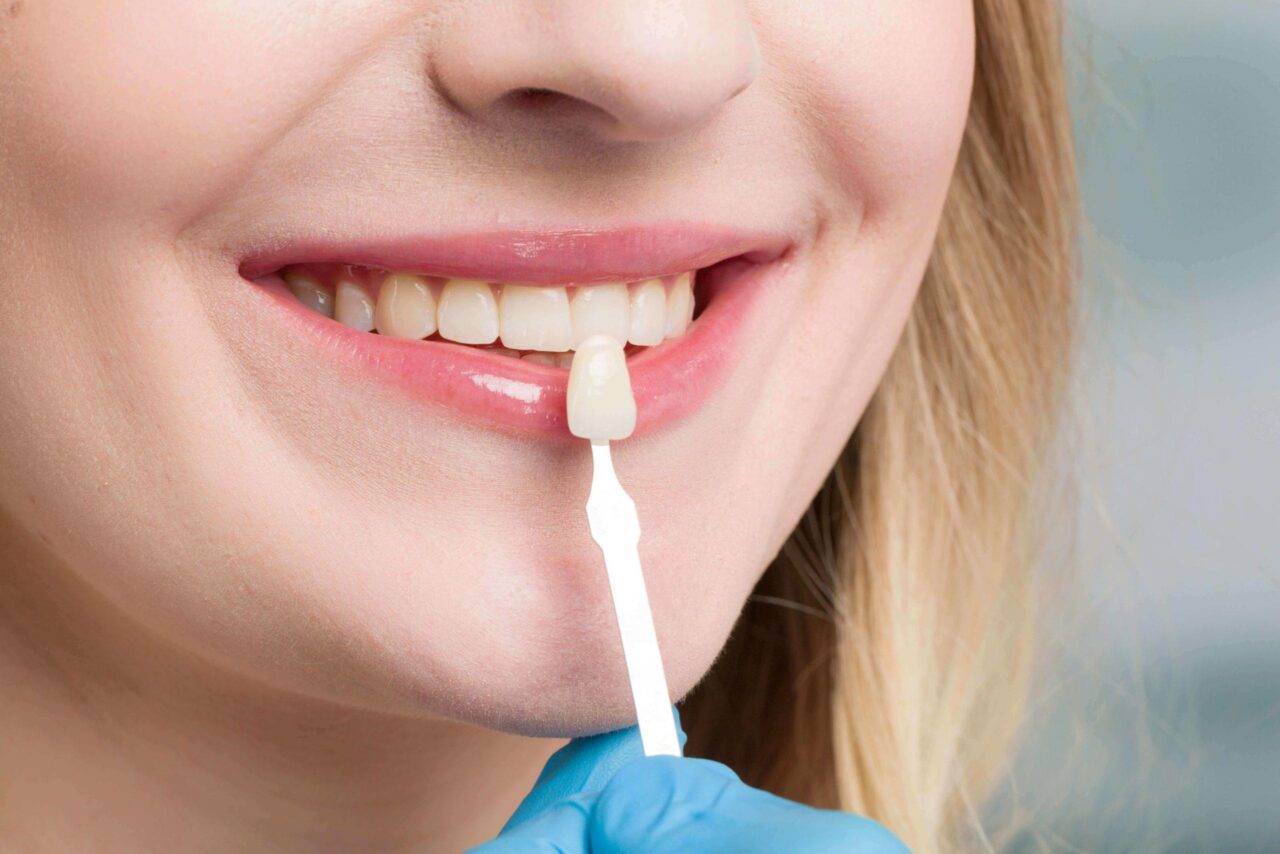
Porcelain Veneers
Porcelain veneers are a way to achieve a million-dollar smile, without having to empty the bank account.
Cosmetic Dentistry
The most common cosmetic dentistry treatment is one that you’re probably already familiar with: Teeth whitening.

Request An Appointment
Dr. Mariana Conant is a Scottsdale-area dentist offering her experience and skill, with a friendly approach to dentistry in order to improve the smiles of her patients.
What Others Are Saying About Us
Dr. Mariana Conant offers her experience and skill, with a friendly approach to dentistry in order to improve the smiles of her patients.


Recent Articles
Our Dentist
Dr. Mariana Conant, DDS is a dentistry practitioner in Scottsdale, AZ and has been practicing for 21 years. She practices dentistry, cosmetic dentistry, and more.
DOCTOR OF DENTAL SCIENCE
Universidade Federal de Goias, Brazil New York University College of Dentistry New York University Esthetic Honors Program Former Assistant Professor in Prosthodontics, Brazil Former Assistant Professor of Esthetics, NYU.
ASSOCIATIONS
American Dental Association, OKU, National Dental Honors Society, Academy of General Dentistry